A Bispecific Monoclonal Antibody Targeting Psl and PcrV for Chronic Pseudomonas Aeruginosa Infection in Patients With Bronchiectasis: Results From a Randomized, Double-Blind Placebo-Controlled Trial (GREAT-2)

Gremubamab in Bronchiectasis: A New Approach to Chronic Pseudomonas Aeruginosa Infection
Rationale:
Pseudomonas aeruginosa airway infection is associated with increased exacerbations and poor outcomes in bronchiectasis. Our prior study (GREAT-1) showed that gremubamab—a bivalent, bispecific mAb targeting Psl exopolysaccharide and PcrV T3SS component—enhanced neutrophil clearance of P. aeruginosa and reduced virulence ex-vivo.
Here we report the efficacy and safety of gremubamab in a proof-of-concept trial in bronchiectasis patients with P. aeruginosa infection.
Clinical Efficacy of Gremubamab in Bronchiectasis
Gremubamab treatment resulted in a significant reduction in bacterial load at EoT (day 84) with the 500mg dose compared with placebo treatment (-1.25 log-CFU (-2.33 to -0.16); p=0.071; ANCOVA), meeting the trial primary endpoint.
A non-significant directional trend was observed for the 1500mg dose (-0.66(-1.71 to 0.39); p=0.2).
The SGRQ was significantly improved versus placebo at EoT (500mg: -10.8; 1500mg: -12.1), and the proportion of patients achieving a clinically significant SGRQ improvement was higher for both gremubamab 500mg (38.5%) and 1500mg (41.7%) versus placebo (8.3%).
Clinically significant benefit in favour of gremubamab treatment at EoT was observed for multiple QoL-B domains.
Impact on Exacerbations and Pulmonary Function
Time to first exacerbation was significantly prolonged at the 1500mg dose versus placebo (p=0.046).
Conclusions – Proof of Concept for Targeted Monoclonal Antibody Therapy
Gremubamab treatment significantly reduced P. aeruginosa airway bacterial load and improved patient-reported quality of life in patients with bronchiectasis, providing proof-of-concept for specific anti-microbial monoclonal antibody therapy.
Authors
M.B. Long, R.C. Hull, A. Gilmour, K. Viligorska, H. Richardson, B.J.M. New, C. Hennayake, R. Galloway, E. Johnson, E. McIntosh, Z. Eke, H. Lind, M. Band, H. Bandara, G. Martin, S. Aliberti, A. Timothy, J. Norwell, J. Whitehouse, C.L. Addy, L. Finney, P. Mitchelmore, S.J. Caskey, R.W. Lord, A.T. Hill, M. Vendrell, E. Polverino, A. Marin, G. Suarez-Cuartin, M.R. Loebinger, M. Tunney, K. Cartwright, R. Hughes, A. Digiandomenico, M.G. Belvisi, W. Brailsford, C. Haworth, O. Sibila, J. Stobo, J.D. Chalmers
Read more details at
Fecha de publicación
Published 2025, 19 May
Categorías asociadas al artículo
Noticias relacionadas
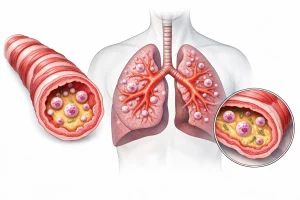
Clinical, molecular and microbial characterisation of the eosinophilic endotype of bronchiectasis: data from the EMBARC-BRIDGE study
Analysis of eosinophilic bronchiectasis exploring airway inflammation, blood eosinophils, microbial associations and disease severity using LC-MS/MS techniques.

Systemic Immune Dysregulation in Patients With Bronchiectasis and Chronic Pseudomonas aeruginosa Infection
Study reveals systemic immune alterations in bronchiectasis patients with chronic Pseudomonas infection, highlighting persistent immune imbalance.

Origenes tempranos de las enfermedades crónicas del adulto
Charla de Alvar Agistí en el H. La Paz sobre los orígenes de las enfermedades crónicas. tempranos en la sesión titulada: Orígenes tempranos de las enfermedades crónicas del adulto. El 24/09/2025

Sputum metagenomics in bronchiectasis reveals pan-European variation: an EMBARC-BRIDGE study
Sputum metagenomics reveals pan-European variation in microbial and resistome profiles in bronchiectasis: an EMBARC-BRIDGE study.

Occluding mucous airway plugs in patients with obstructive lung diseases: a new treatable trait?
Airway mucous plugging is associated with exacerbations, lung function decline, and mortality in COPD, asthma, and bronchiectasis. Identifying it as a treatable trait may improve patient outcomes through airway clearance techniques and pharmacological strategies.
Falling through the cracks: what happens to survivors of preterm birth?
Survivors of preterm birth face increased risks of respiratory diseases, yet awareness among specialists is low. This study examines gaps in long-term care, highlighting the need for clear follow-up guidelines and improved communication between medical teams.
Imagen desarrollada ChatGPT y adaptada con Canva
