Occluding mucous airway plugs in patients with obstructive lung diseases: a new treatable trait?

Airway Mucous Plugging in Chronic Airway Diseases
Chronic mucous hypersecretion (CMH) is a well-known feature in several obstructive lung diseases, including asthma, COPD, and bronchiectasis. In COPD, it accelerates lung function decline and increases exacerbation frequency. Similarly, it affects 25% of asthma patients and is linked to lung function impairment and exacerbations.
Bronchiectasis often coexists with COPD, appearing in 30% of cases and contributing to chronic infections and worse outcomes.
Additionally, eliminating Pseudomonas aeruginosa colonization in COPD improves prognosis.
They suggest that airway mucous plugging can be viewed as a novel treatable trait (TT) in patients with chronic airway diseases.
Treatment Strategies for Airway Mucous Plugging
Current evidence suggests that airway clearance techniques can effectively improve sputum clearance, reduce symptoms, and lower exacerbation frequency in COPD and bronchiectasis.
Additionally, pharmacological interventions, including mucolytic agents like N-acetylcysteine (NAC), have shown promise, particularly in targeted subgroups.
Other therapeutic strategies, such as modifying mucin biosynthesis, interfering with mucus structure, and targeting ion channels, are under investigation.
Biological treatments like tezepelumab and dupilumab, initially developed for asthma, have also demonstrated potential in reducing mucous plugging severity and are now being considered for COPD patients with a T2 trait.
The Role of Airway Mucous Plugging in Personalized Medicine
Identifying mucous plugs via chest CT should be integrated into the clinical evaluation of chronic airway disease patients as a potential treatable trait.
The growing emphasis on precision medicine is leading to significant advancements in the management of chronic respiratory diseases.
Authors
Alvar Agustí, Stefano Aliberti, Francesco Blasi, Marc Miravitlles, Alberto Papi
Read more details at
Fecha de publicación
Published online 27 January 2025
Categorías asociadas al artículo
- Asma-Asthma, Bronchial infection-Infección bronquial, Bronchiectasis-Bronquiectasia, Comorbidity-Comorbilidad, COPD-EPOC, Emphysema-Enfisema, Estudios-Studies, Exacerbations-Exacerbaciones, Farmacología-Pharmacology, Lung function-Función pulmonar, Rasgos tratables-Treatable traits, Tratamientos-Treatments
Noticias relacionadas
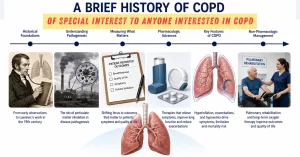
A Brief History of COPD: As Told by Some of Its Senior Scientists and Clinicians
Explore the history of COPD and the evolution of disease concepts, treatment strategies, patient outcomes, pulmonary rehabilitation and clinical management.

Climate change and respiratory health: implications for respiratory clinicians in primary and specialist care
How climate change affects asthma and COPD, the role of air pollution and inhalers, and why sustainable respiratory care matters for patients and clinicians.

Indoor radon exposure and COPD in never smokers: a case–control study in a radon-prone area in Spain
Study on indoor radon exposure and its association with COPD risk and severity in never smokers in a radon-prone region.
Imagen desarrollada DALL·E y Canva
