COPD Management in Primary Care: Underutilisation of Nursing Consultations

COPD Primary Care Nursing and Healthcare Utilisation Overview
COPD Primary Care Nursing and Healthcare Utilisation Overview
To describe the clinical profile, comorbidity burden, follow-up and healthcare utilisation in patients labelled as having Chronic Obstructive Pulmonary Disease (COPD) in Primary Care (PC) nursing consultations.
Design: Real-world data COPD, retrospective, observational study using routinely collected data in electronic health records (EHR).
This study adheres to the STROBE reporting guidelines for cross-sectional studies.
Patient Characteristics and Data Collection in COPD Management
All patients aged ≥ 15 years with a recorded diagnosis of COPD in their EHR, excluding institutionalised individuals and those deceased before study onset.
Final sample: 474 patients (105 women, 369 men; mean age 70 years) from a reference population of 28,000 individuals.
Main measurements
Data included socio-demographics, smoking/alcohol, mMRC dyspnea, inhaled therapy/adherence, spirometry, comorbidities, Adjusted Morbidity Groups (GMA), active COPD care plans and 12-month healthcare use.
Key Findings on COPD Nursing Consultations and Comorbidities
EHR showed a high rate of missing data in follow-up variables (inhaler adherence 28.5%; dyspnea 17%-20%).
Despite that, all participants were ‘labelled’ as COPD, most of them lacked spirometric confirmation. Active smoking was highly prevalent (52.3% women, 45.0% men). Hypertension, obesity and osteoarthritis were the most common comorbidities; anxiety, depression, osteoporosis and thyroid disorders were more frequent in women.
Higher GMA complexity correlated with more Primary Care visits, especially nursing consultations, particularly in patients with cardiovascular disease and diabetes (p < 0.001) for 12 months follow-up.
Conclusions on Improving COPD Care Through Nursing
EHR-labelled COPD patients with cardiometabolic comorbidity received more structured nursing follow-up and more annual visits than without. Improving EHR recording, integrating spirometry with the EHR, and prioritising high-complexity profiles could enhance monitoring, treatment optimisation and equity-nursing consultations are a key lever.
Authors
Marc Vila, Meritxell Mondejar, Sergio Cazorla-Calderón, Àngels Ballarin, Sandra Casas-Recasens, Rosa Faner, Alvar Agustí
Read more details at
Fecha de publicación
2026 Feb 12
Categorías asociadas al artículo
Noticias relacionadas
Climate change and respiratory health: implications for respiratory clinicians in primary and specialist care
Review on climate change and respiratory health, focusing on chronic respiratory diseases and implications for primary and specialist care.

Personalizing COPD care: phenotypes, endotypes, GETomics, the the trajectome, syndemics and treatable traits
Discover how personalized COPD care integrates phenotypes, endotypes, GETomics, trajectome, syndemics, and treatable traits to improve patient outcomes.

TED Talk – The Invisible Epidemic
Jean Wright presents at TEDxCharlotte how millions live with COPD unknowingly. It’s time to identify and help the “missing millions.”

Climate Change & COPD: A GOLD Science Committee Review
Climate change and COPD are linked through extreme temperature, wildfire smoke, dust storms and allergen exposure, which pose major health threats.

Artificial Intelligence in COPD
Artificial Intelligence in COPD is transforming disease management, from underdiagnosis to treatment guidance. Discover how machine learning clusters patients, predicts outcomes, and optimizes healthcare resources.
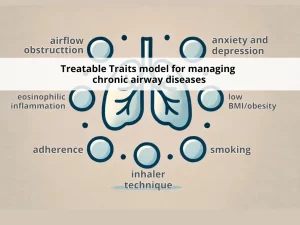
Change is in the air: key questions on the ‘Treatable Traits’ model for chronic airway diseases in primary care
Explore Treatable Traits model for chronic airway diseases like asthma and COPD in primary care. Learn about seven key traits — airflow obstruction, eosinophilic inflammation, adherence, inhaler technique, smoking, low BMI/obesity and anxiety and depression — that guide personalized care.
Imagen desarrollada con ChatGPT
